
These Houston Doctors Seek to Diagnose the Previously Un-Diagnosable
Nine-year-old Blaine Tunning is blind. He suffers from cortical vision loss, a problem with his brain, not his eyes, which are healthy. Still, when his father David and mother Casey talk about the ordeal the family’s undergone the last three years, the boy’s eyes unflinchingly follow whichever parent is speaking.
Towheaded and spirited, Blaine is the picture of an all-American boy, if one a bit younger than he is. He’s small in size, more in line with a well-proportioned 6-year-old. Until he had his first seizure in May of 2014, Blaine’s parents never suspected he was anything but normal. Then, two months later, “he had a seizure and lost his vision and his memory,” recounts David, who says his son’s continued trouble with short-term memory makes learning in school all but impossible. The couple rushed their child to the ER, where imaging revealed that Blaine’s brain was severely calcified and that there was profound trauma to the gray matter. “We realized immediately that we were dealing with something big,” David recalls.
At the time, Casey was a nurse. Today she devotes her time to researching Blaine’s mysterious condition—and awaiting the next call from school informing her that her son has had yet another seizure. “Your life revolves around it,” says Casey. The past three years have been a roller-coaster of doctor visits and unconfirmed opinions about what she calls “the little monster” that has snatched her son.
But in one way, the family is lucky: The Tunnings live in Montgomery, not so far from Houston. Here, Baylor College of Medicine and Texas Children’s Hospital are working together as one of the seven clinical sites, and one of only two DNA-analysis facilities/model-organisms-screening centers—where animals with patients’ genetic mutations are made and studied—in the international Undiagnosed Diseases Network (UDN), making it the best-equipped site in the nation. For those who qualify, the network can give answers to families who have lived with years of uncertainty.
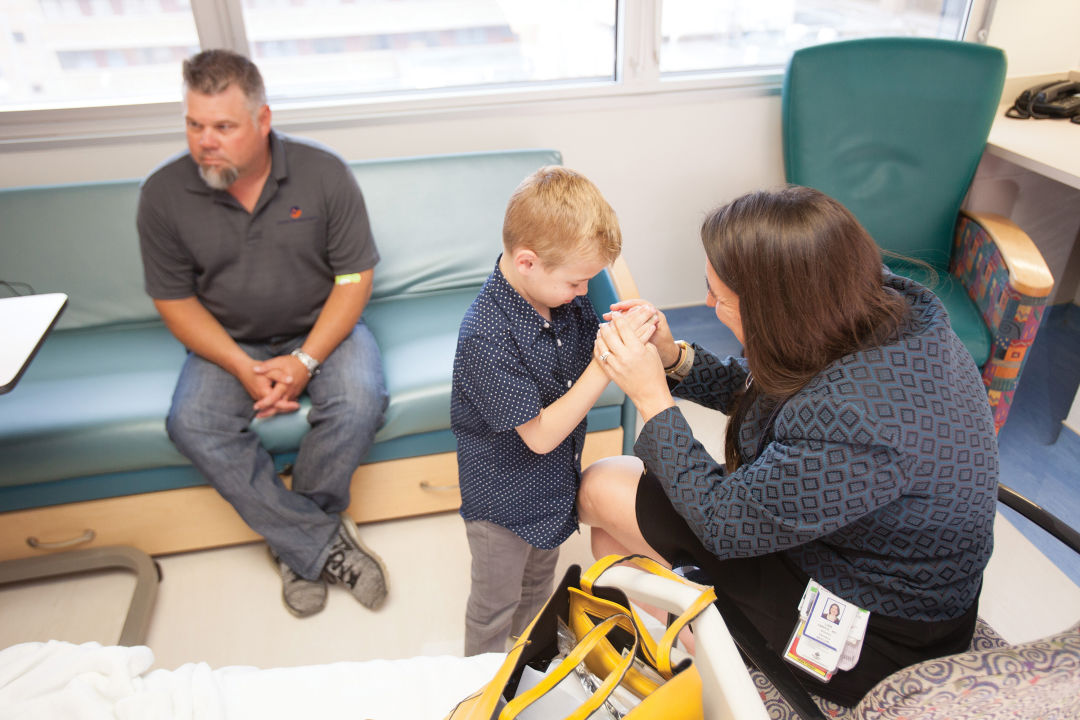
Blaine Tunning with Lisa Emrick
Image: Daniel Kramer
The Houston UDN site—which exists in the offices of Baylor’s genetics department, labs at Texas Children’s, and hospital rooms wherever patients can be best served—got its $7.3 million, four-year grant from the National Institutes of Health in 2014, the same year Blaine had his first seizure. Brendan Lee, the chairman of molecular and human genetics at Baylor, is the principal investigator and, along with lead coordinator Jill Mokry and their team, evaluates about 50 patients each year, who must provide proof that typical doctors and tests have not been able to produce a diagnosis. About two thirds of those are children.
The application process is reminiscent of trying to gain entry to a selective college: Besides a painstaking medical history and letter of recommendation, prospective patients must provide everything from videos and photos to pathological slides and reports. Some patients are turned away because the team isn’t confident it can help and doesn’t want to offer false hope. Others are diagnosed during the screening process, when the UDN doctors’ expertise in rare diseases helps them to solve mysteries that have confounded others. Roughly half of the applicants are eventually accepted.
Of course, Lee’s team made diagnoses frequently before joining together in the UDN. How is what they’re doing here different? Though they’ve always been engaged in gene discovery, the network’s funding provides resources for clinicians to dig deeper and even perform research on each patient. “Rare diseases as an aggregate affect 30 million Americans,” says Lee. That means research can help a great number of people with uncommon maladies, but also teach researchers about genetics that affect us all.
Some of the most probing work performed at the Houston UDN site uses other life forms—specifically fruit flies and zebrafish—to solve patients’ medical problems. The process begins with doctors sequencing patients’ genes in hopes of identifying genetic mutations. If an anomaly is isolated to a single gene—a Mendelian disorder—then it’s easier to study, and clinicians are more likely to find answers.
“It essentially provides a way for us to study genes and variants that are identified from the genomic sequencing of undiagnosed patients,” explains pediatrician and medical geneticist Michael Wangler, who often can be found in a lab at the Model Organism Screening Center, surrounded by sealed test tubes filled with fruit flies—or drosophila, as he prefers to call them.
When doctors want to find out whether a patient’s mutation is the cause of their symptoms, that patient is often a good candidate for an animal-model study. “There’s no good way to find out without making a model and seeing if the variant changes the function somehow,” Wangler says.
In this way, the team has been able to identify several new genetic diseases. One model organism still being studied produced a syndrome so quickly that the mutation of CACANA1A has already seen publication. Now knowing to look at that particular gene, Mokry searched back through records and quickly found four more instances of patients whose conditions have the same cause. For them, it could mean a long road ahead, but at least doctors know exactly what they’re battling.

Carol Gross and Amy Rowland at home.
Image: Daniel Kramer
Though Baylor and Texas Children’s are the primary sites of the UDN in Houston, visits also happen at CHI St. Luke’s Health, which is part of the Baylor family. And the network extends far beyond those hospitals’ walls. Not only is the wider Houston medical establishment growing increasingly conscious of the work the UDN can do for its patients, patients are flown in to meet with its doctors from across the country.
In 2016, Dr. William Ondo, a neurologist at Houston Methodist, recommended that Carol Gross apply to the network for her daughter, Amy Rowland. Born in 1969, Rowland was always different. When she was a small child, she learned only a few words before losing the ability to speak. She also developed a kidney and bladder infection that led doctors to discover that she had only one kidney, which was misplaced in her abdominal cavity. “Life went on, and we lived our lives, and we watched her grow, and she was very slow in developing, but she was precious and cute,” Gross recalls. “Everybody cherished Amy.”
Doctors wouldn’t commit to saying whether Rowland was mentally challenged; in fact, they never gave a name to her problems. The closest thing the family ever got was the phrase “multiple congenital anomalies,” which hinted that the doctors knew it was a genetic disorder.
Ondo worked to improve Rowland’s life and, over time, referred her to a number of studies, but they were all dead ends. Then Gross applied to the UDN, and Rowland was accepted. When the lab sequenced her genes, doctors discovered a mutation in the gene DDX3X. The timing for the diagnosis couldn’t have been better. The first paper describing the condition, also known as DDX3X, had been published the previous year.
DDX3X causes intellectual disabilities and other congenital anomalies in females, including similar facial features—the same cute, pixie-ish look that Gross describes when discussing her daughter’s charms. As of press time, there are 95 known cases in the world. Mokry says Rowland “is the oldest person that we know of with this diagnosis, providing some possible insights about prognosis for others.”
Gross never asked the UDN doctor the question she was afraid to verbalize. Still, she recounts, “he did say, ‘It’s nothing you did or your husband did.’ He volunteered it. I guess he knew from other people that it may be an issue that’s worrisome on your mind.”
Today, Rowland lives in a group home in Friendswood and spends weekends with Gross. From time to time, she heads to Houston for continued testing at Baylor’s neurogenetics clinic. While new discoveries probably won’t mean changes for Rowland, that’s fine with Gross. “She’s quite a character,” she says of her daughter. “She’s funny. She’s lovable. She loves her family. Amy is who she’s supposed to be.”

Blaine's parents help Emrick measure his arm span.
Image: Daniel Kramer
When Lee accepts a patient to the Undiagnosed Diseases Network, he and his team discuss which holes need filling: tests that need to be done, doctors who might have insight. In Blaine’s case, neuro-geneticist Lisa Emrick was an obvious fit. Emrick is known as the “Zebra Doctor” among her colleagues for her ability to see rare diagnoses—zebras—where others might only think of the more common “horses.”
It was Emrick’s eleventh and twelfth fingers, an inheritance from her father and grandfather, that created her interest in genetics. They’re gone now, and she’s the medical director of neurogenetics for Texas Children’s, perhaps the country’s only specialist in neurodevelopmental disabilities with training in neurology, pediatrics and genetics.
It’s no big surprise she might be the one to crack the case of Blaine Tunning. “I see the rarest of the rare,” she says. “My whole clinic is filled with the most interesting patients.” The zebras.
While Emrick knows that she and the rest of the team are unlikely to find an answer immediately, she has leads. Blaine has a 20-year-old brother with a similar, though far less severe, collection of neurological symptoms. No other doctors had thought to test him until now to see whether the two share genetic mutations that might make it easier to identify a condition.
Emrick has a hunch that Blaine may have an atypical presentation of the rare Aicardi-Goutières syndrome. First identified from a pool of eight cases in 1984, the inflammatory disorder causes symptoms similar to his. There are the flare-ups. The calcification. The cognitive issues, such as the severe short-term memory loss that makes school a challenge.
Blaine isn’t a textbook case, however. While Emrick usually associates Aicardi-Goutières with muscular issues and movement disorders, the boy’s motor skills are almost normal, and he has no complaints of involuntary movements. It will take time to get a more definitive answer—or at least another hint in the right direction.
If Blaine’s condition does turn out to be Aicardi-Goutières, the good news is that there are drug trials currently underway. And though his case isn’t exactly typical, Emrick always has it in mind that the same disorder can look different in every patient. She says she’s seen at least five patients with Aicardi-Goutières, which is so rare, it’s unknown how many people in the world have it. “You might share one mutation, but there’s like 25,000 other genes,” she explains.
Whatever happens, the UDN will continue to work to solve Blaine’s case, although Emrick cautions that the answers might not be satisfying ones. “When we’re talking about these conditions, some of these answers are not great answers,” she acknowledges. But the study of rare diseases often helps to create better understanding of other, less esoteric disorders, enhancing the potential for far-reaching medical discoveries.
As for the Tunnings, David says he just hopes the doctors can help prevent Blaine from deteriorating further. And Casey says they will go to the ends of the earth to do what they can for their zebra child. “You just don’t give up,” she says. “You keep on grinding and live every day to the fullest.”













































